The final stages of life are often accompanied by natural but misunderstood phenomena. These moments can be intimidating, stirring fears and misconceptions among families witnessing their loved ones in their last hours.
Hospice Nurse Julie sheds light on these occurrences in a YouTube video, particularly focusing on the “death rattle,” a common yet startling event. By understanding these natural processes, we can hopefully have a bit more peace and clarity for those navigating this challenging time.
What Is the ‘Death Rattle’?

The “death rattle” refers to terminal secretions experienced by many at life’s end. It’s characterized by a specific sound resulting from saliva and secretions accumulating in the throat, as the dying person can no longer swallow effectively.
This might sound alarming. “Many people think their loved ones are suffering, but it’s actually a little bit of secretion in their loved one’s mouth,” hospice nurse Julie said in her YouTube video.
Misconceptions Debunked

A common fear is that the dying individual is in pain or drowning due to these sounds. This misconception can cause unnecessary distress for families.
However, the truth is less grim: “People think their loved ones are drowning when in reality all it is is a little bit of secretion,” Julie says.
Why Does It Happen?
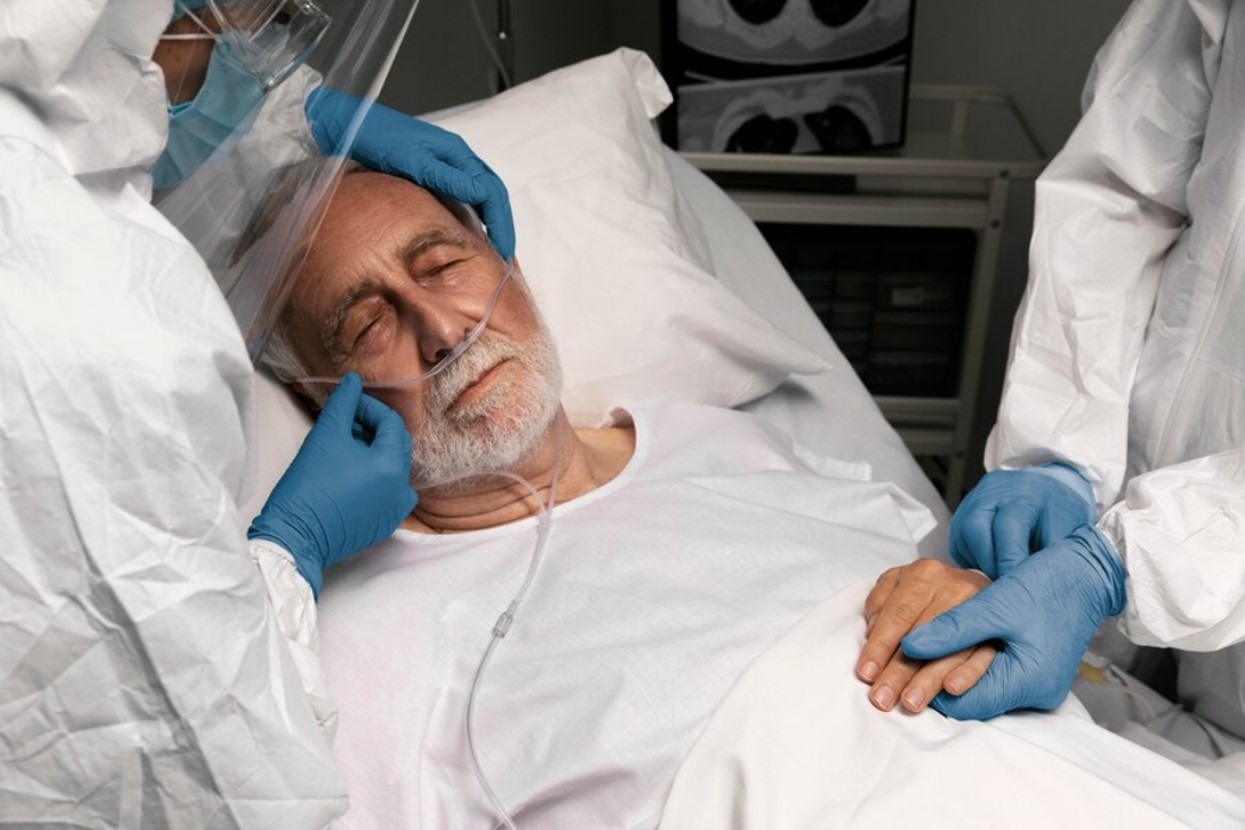
At life’s end, natural bodily functions begin to slow down, including the reflex to swallow (via Palliative Care Australia). Although saliva production continues, leading to accumulation in the mouth, this is not a sign of distress but rather a part of the body’s final processes.
This can lead to the characteristic “death rattle” sound, which, while disturbing to some, indicates no discomfort for the dying individual.
Addressing the Sound
The “death rattle” can be unsettling, but understanding its nature can help alleviate concerns. While the sound is noticeable, it does not indicate suffering.
Knowing this can help those at the bedside focus on comfort and presence rather than unnecessary worry about pain or distress.
What Can Be Done?

There are ways to manage the “death rattle” to make the environment more peaceful for both the patient and their loved ones. Positioning the patient can help, as can certain medications, although they might lead to dry mouth.
As Julie puts it, “I’m not particularly into the medication because it gives the loved one dry mouth.” These measures are aimed at comfort, not cure, reflecting the palliative nature of end-of-life care.
Changes in Breathing Patterns
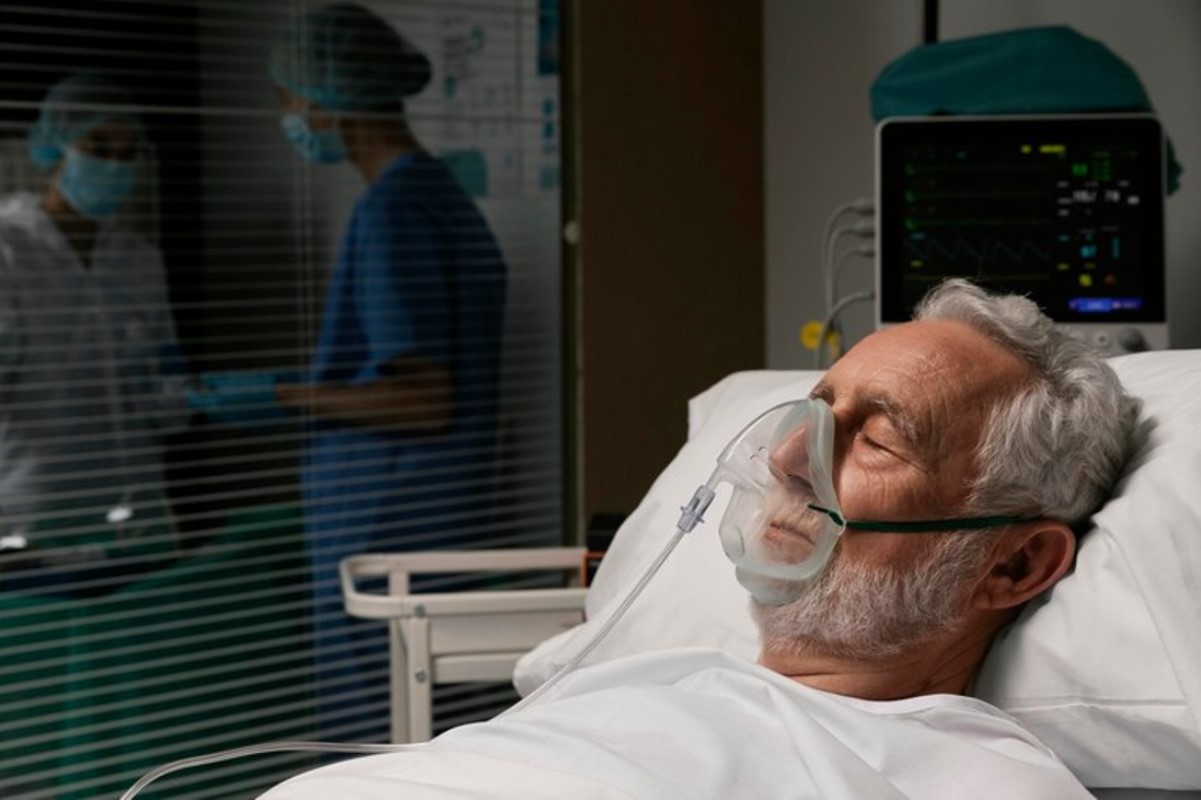
Alongside the “death rattle,” breathing patterns often change dramatically in the final stages of life. This shift is normal and expected, part of the body’s natural slowing down.
“This is literally expected and normal and will happen with everybody,” says Julie. Recognizing this as a natural part of dying can help families prepare and understand what to expect.
Recognizing Comfort in the Dying
Understanding the signs of comfort in a dying person is crucial. Just like infants, who cannot communicate their needs verbally, “Dying people are like babies. We know if they’re okay versus not okay by how they look and how they act.”
This perspective can help families gauge their loved one’s comfort level without verbal communication.
Medical Perspectives

Health care professionals use various nonverbal indicators to assess a patient’s comfort at the end of life (via Hospice of the Northwest).
By observing facial expressions, body language, and response to touch, they can infer whether the individual is at peace or in distress.
Educating Ourselves and Others

Education about the dying process can transform a fearful experience into one of understanding and acceptance.
“The more we know, the less you fear,” Julie says on YouTube. By demystifying the end of life, individuals can approach these moments with less anxiety and more focus on sharing love and support.
Creating Beautiful Moments

Armed with knowledge and understanding, families can create peaceful, meaningful final moments with their loved ones.
Instead of focusing on medical interventions or signs of distress, they can concentrate on expressing love, sharing memories, and offering comfort — transforming a time of fear into one of connection and closure.
Continuing the Conversation
The journey doesn’t end here. Continual learning and conversation about end-of-life care can empower more individuals to face these moments with grace and knowledge.
By fostering a broader understanding, we can all contribute to a culture that approaches death with respect, empathy, and dignity.








































